HIE and Autism - Is it Necessary to Pick One or the Other?
This article is available as a PDF here.
It a recent case of ours, a treating child neurologist diagnosed autism in our 11-year-old client who was clearly a victim of obstetrical negligence and resultant HIE - manifested by profound delays in verbal communication, cognition and behavior. Defense counsel seized the day and took that neurologist’s deposition (but not any of the child’s other specialists who had diagnosed the child as having the sequala of HIE). The first several hours of the deposition focused on the neurologist confirming, re-confirming and then re-re confirming the diagnosis of autism. Defense counsel then attempted to lead the neurologist into the conclusion that autism has no known etiology. The neurologist shocked Defense counsel and responded, “Are you kidding?” and then went on to describe how this child’s birth presentation was classic for severe asphyxia and clearly demonstrated the cause of what she had labeled as autism.
So in this case, our young client’s treating physician did our work for us, but more typically, we are left to unravel the often intentionally confusing label of autism rather than HIE - whether diagnosed by treater or by defense expert. The defense argument goes, “Since autism is of unknown etiology, no one can credibly say, as the plaintiffs are in this case, that the minor-plaintiff’s deficits are related to a duration of perinatal asphyxia and HIE.”
Autism v. HIE
Autism has historically been diagnosed with a constellation of symptoms that did in fact distinguish the condition from an injury caused by birth asphyxia; however, that historic label of autism has evolved. A comparison of the former and latter diagnostic criteria reveals that today’s autism diagnosis encompasses far more symptomology than in years past. Indeed, what is now labeled as autism most certainly includes the classic sequala of HIE.
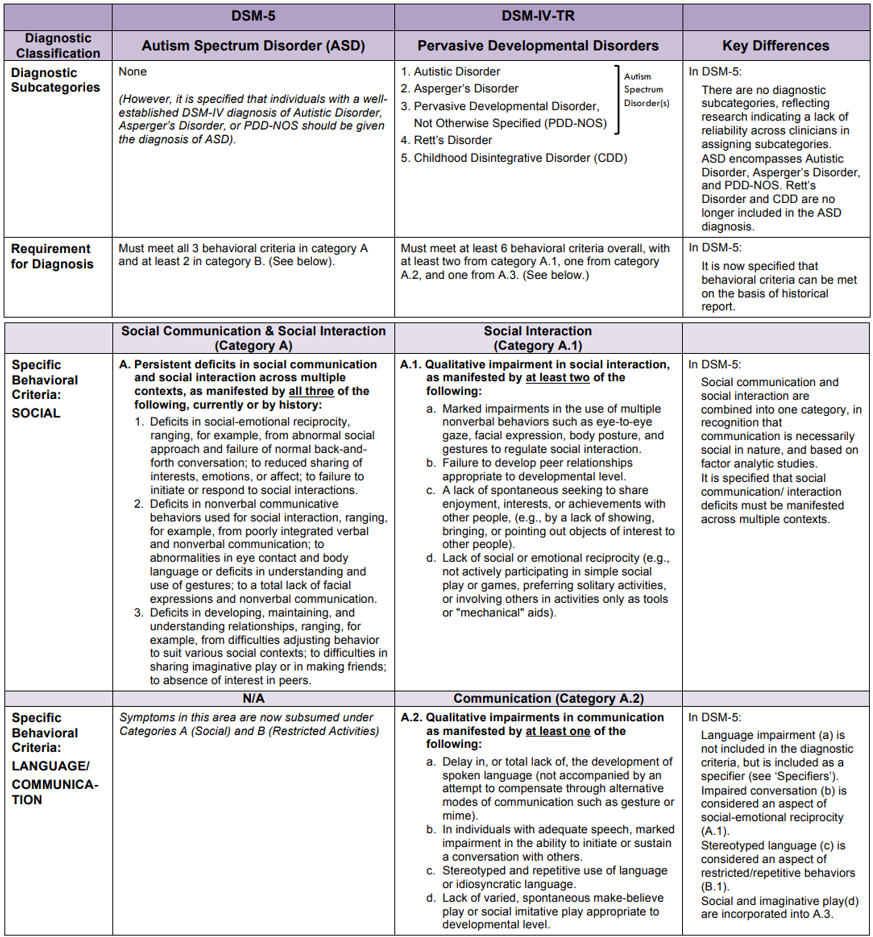
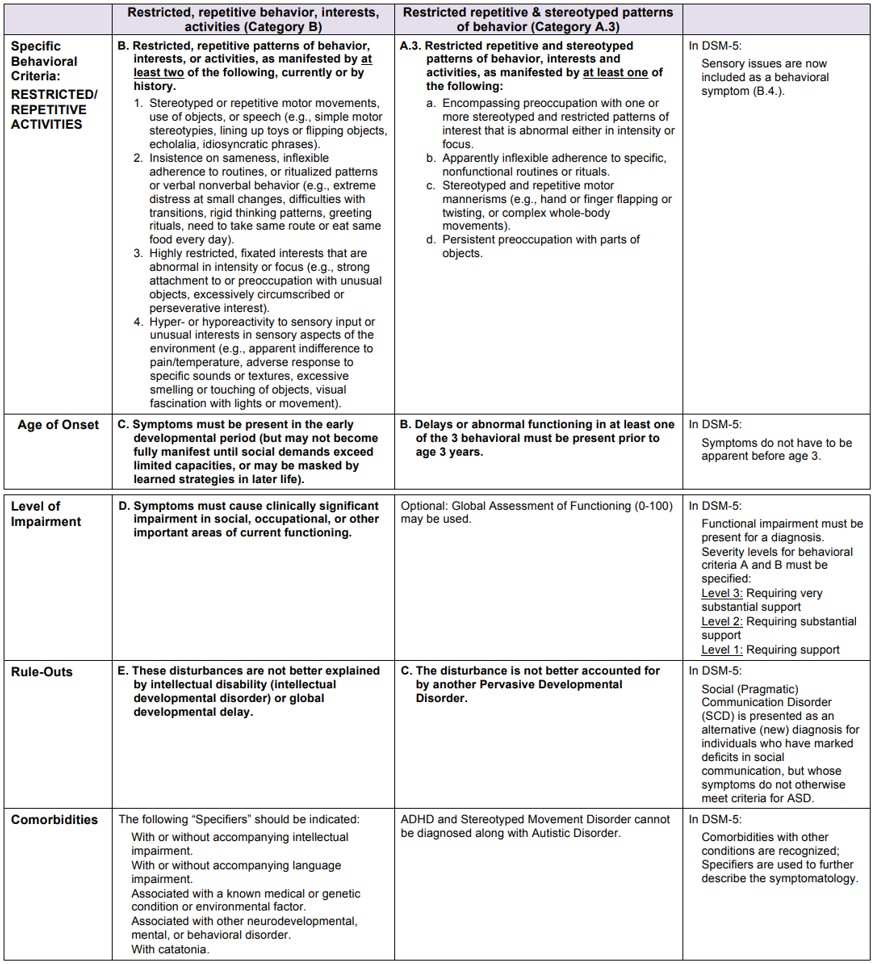
Autism Spectrum Disorder (“ASD”) can have mild to severe symptomology that presents itself in a variety of areas. Unfortunately, there isn’t a blood test or imaging study that can definitively diagnose someone with ASD. As such, we must rely on skilled providers to use subjective and objective testing and criteria to determine if our clients can be categorized on this spectrum. The table below demonstrates the changes between the DSM-IV-TR (1994) and the DSM-5 criteria (2013) as laid out by Collen M. Harker, M.S. and Wendy L. Stone, Ph.D of University of Washington READi Lab.
Comparison of the Diagnostic Criteria for Autism Spectrum Disorder Across DSM-5, 1 DSM-IV-TR, 2 and the Individuals with Disabilities Education Act (IDEA)3 Definition of Autism
- Colleen M. Harker, M.S. & Wendy L. Stone, Ph.D. University of Washington READi Lab
So while it is true that there is no known definitive causation for ASD, there are many factors that are associated with an ASD diagnosis. Most studies, since the arrival of the DSM-5, support that ASD criteria is more restrictive than the previous DSM-IV. However, with our HIE clients, their previous HIE diagnosis is now considered in the ‘Comorbidities’ section of the DSM-5. This section recognizes that comorbidities, such as HIE, can be associated medical factors of ASD.
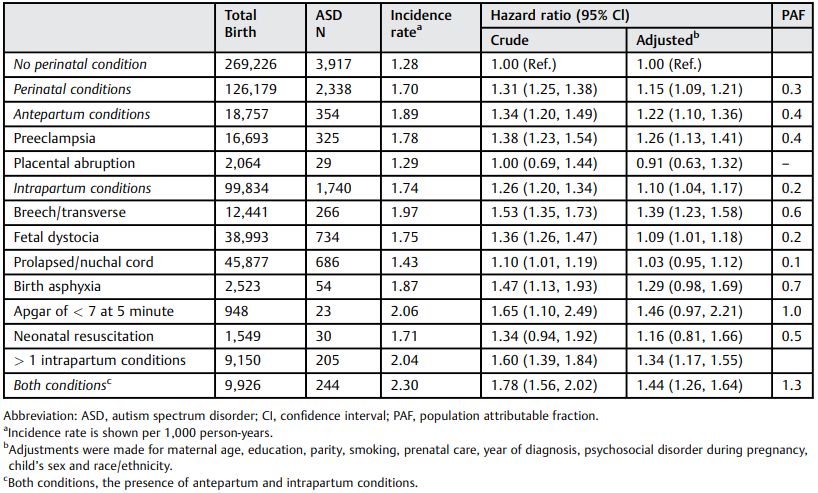
Note also that there is now an academic grounding in the assertion that HIE, among other conditions, can cause the deficits now labeled as autism. The American Journal of Perinatology published an article in 2017, Association of perinatal risk factors with Autism Spectrum Disorder. This was a retrospective cohort study of 594,638 children’s medical records to determine perinatal complications and diagnosis of ASD (DSM-IV). The table below shows the association between perinatal conditions and ASD. There is a clear increase in diagnosis of ASD with birth asphyxia and higher still with APGAR of <7 at 5 minutes. The most significant indicator is related to having both antepartum and intrapartum conditions. The DSM-5 is still too new for use in large scale retrospective studies, such as this one.
This study demonstrates the significance of perinatal conditions that contribute to HIE and associated increases in the diagnosis of ASD in childhood. It serves to aid in the establishment that HIE and ASD are associated; and it gives cause to encourage early monitoring and identification for ASD rather than feeling the need to work around a diagnosis of ASD.
So whereas the tendency in our cases has been to fight the diagnosis of autism, there should no longer be that need. Our experts should be armed and able to explain that ASD is a multifaceted and complex diagnosis, encompassing a broad constellation of symptoms for which there is academic consensus that HIE is a cause. Stated differently, what we are now calling “autism” is what a consensus of physicians used to agree was classic HIE (and still should).